In this article Dr. Thomas Zumstein presents a Neoss implant case that has been in function for more than 11 years. The case shows that long-term success and stable bone levels can be achieved in a predictable way with a high level of simplicity using the Neoss implant system.
The clinical case is part of a previously published long-term study population on Neoss implants. The five year data from the study (Zumstein 2012) showed an overall survival rate of 95.0% and an average marginal bone loss of 0.4 mm during the first 5 years in function. These results indicate predictable treatment with good clinical outcome and stable bone levels after 5 years in function. The study has now been followed up for 10 years with no additional failures and no further bone loss since the 5-year follow-up.
Case background
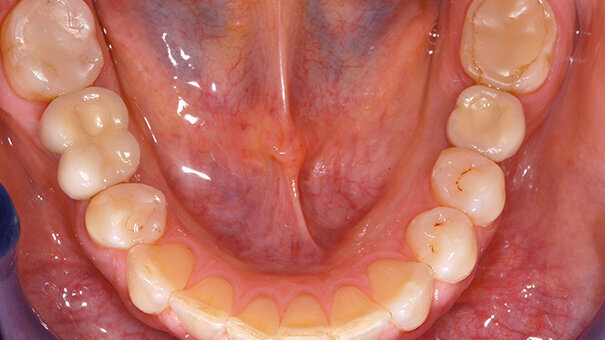
A 41 year old woman came to our clinic with missing first molars on both sides of the mandible (Figure 1). The patient was healthy, with a good oral hygiene, she was a non-smoker and with good compliance. This made her a good candidate for implant treatment.
The main challenge in this case was the large space in the right molar area (position 46). The question in such case is whether to place one or two Implants, and in which positions to place them.
In such cases, if excellent implant stability can be obtained, I prefer to place one implant in the distal socket and the restoration with a crown with a mesial cantilever. I prefer this for several reasons:
- Smaller space between implant and adjacent teeth
- Less food impaction
- Better possibility to maintain a good oral hygiene
- Better esthetics: “more tooth than tulip“
- Better economic value for the patient
One risk with this approach is unfavorable load conditions due to the cantilever. Therefore it is crucial to ensure that the implant stability is high and that the occlusal loads of the cantilever are minimized. In addition there are a few additional considerations I make when planning for a cantilever:
- The natural tooth next to the cantilever is very important. It provides sensory feedback and minimizes the risk of overloading the cantilever when biting.
- The cantilever should always be on the mesial side, since the bite forces are higher on the distal side of the reconstruction.
- The patient should not have any periodontal problems. If the patient is missing many teeth, the bite forces on each unit is increased and thereby the risk of overloading the cantilever is increased.
- Implant placement
Two Neoss 4.0 x 11 mm implants were placed, one implant was placed in the left first molar area and another in the right first molar area. A distal position was chosen in the right first molar area, correct position and direction was ensured during drilling using a direction gauge (Figure 2). The implant was placed in a slight supracrestal position (Figure 3).
If you have good keratinized soft tissue and you can place the implant as shown, then bone augmentation (GBR) is not necessary. In this case a cover screw was placed (Figure 4) and the implant was submerged during the healing period.
It is crucial to place the implant with a good primary stability and to obtain correct position and direction of the implant, in order to assure controlled loads and that the implant can be easily restored with a screw retained reconstruction.
Healing protocol
The implants were allowed to heal submerged for 12 weeks. After reopening, PEEK healing abutments were connected to the implants (Figure 5) and the soft tissue were allowed to heal for an additional 2 weeks before impression taking.
Impression taking
After soft tissue healing, impression copings were connected to the implants (Figure 6 and 7), note the good position and direction of the implants.
I recommend to always use an open impression tray. The reposition of the implant replica is much easier for the technician. The impression tray was modified with access holes that matched the implant positions (Figure 8). Extension tubes were mounted on the impression copings and an impression was taken (Figure 9).
Prosthetic workflow
The lab created cast, wax up frameworks in gold (Figure 10) on Neolink abutments. The final crown was a gold ceramic screw retained single crown (Figure 11). Note the tight contact between the crown and adjacent teeth, both mesially and distally.
Prosthetic delivery
At time of prosthetic delivery, the PEEK healing abutments were disconnected and a healthy soft tissue around the implant was revealed (Figure 12).
The definitive prostheses were tried in (Figure 13 and 14). Articulating foil was used to avoid direct occlusal contacts. The screw access holes were closed after try in and delivery (Figure 15). Good contact of the screw retained implant reconstruction to the adjacent teeth is important to avoid food impaction. The cantilever must be able to clean with super floss or at least with inter dental brushes.
Long-term follow-up
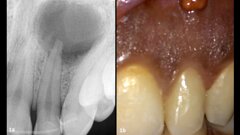
Figure 16 and 17 show the clinical situation after 11 years. Note how stable the soft tissues have remained over time. The bone levels also remained stable over the entire 11 years. Figure 18-21 show baseline and 11 year radiographs of both reconstructions. Note how the bone levels are slightly higher after 11 years than at time of impression.
Conclusion
This case shows that long-term stable bone and soft tissue levels can be achieved in a simple and predictable manner using the Neoss implant system.
References
Zumstein T, Billström C, Sennerby L. A 4- to 5-year retrospective clinical and radiographic study of Neoss implants placed with or without GBR procedures. Clin Implant Dent Relat Res 2012;14(4):480-490.
Neoss was founded in 2000 by CTO, Fredrik Engman and Professor Neil Meredith and is head quartered in Harrogate, North Yorkshire, in the United Kingdom. The...
Dental Tribune MEA had a pleasure to speak with Dr Robert Gottlander who is President and CEO of Neoss. With over 40 years of dental industry experience, ...
Live webinar
Wed. 3 June 2026
9:00 pm UAE (Dubai)
Live webinar
Thu. 4 June 2026
10:00 pm UAE (Dubai)
Live webinar
Mon. 8 June 2026
8:00 pm UAE (Dubai)
Live webinar
Mon. 8 June 2026
9:00 pm UAE (Dubai)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
10:00 pm UAE (Dubai)
Live webinar
Wed. 10 June 2026
7:00 pm UAE (Dubai)
Live webinar
Wed. 10 June 2026
10:00 pm UAE (Dubai)
Nacho Fernández-Baca DDS, MSc



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس











































To post a reply please login or register