Implant dentistry has evolved dramatically in the 50 years since Branemark’s first patient was treated. The combination of improved micro-roughened implant surfaces and tapered implants offers both enhanced initial primary stability and more rapid osseointegration. This has led to successful treatment of many patients in an accelerated protocol, often offering early or even immediate restoration of the implants.
Those who have become involved with implants in the last few years may take this early or immediate loading for granted, and consider it to be the norm for most patients; however only by careful case selection can we ensure predictable success.
Some patients however present with a complex mix of problems that necessitate a slower, systematic approach to implant treatment if optimum results are to be achieved. Professor Dennis Tarnow of Columbia University, one of the world’s leading implant specialists, has a well used maxim… “Let’s do one miracle at a time”. The purpose of this article is to present one such case when only by a stage by stage systematic approach was a good result achieved for the patient.
Case Report
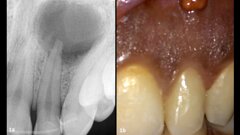
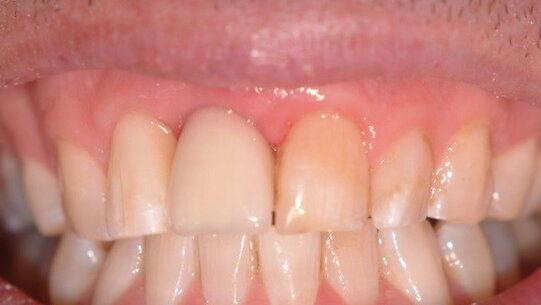
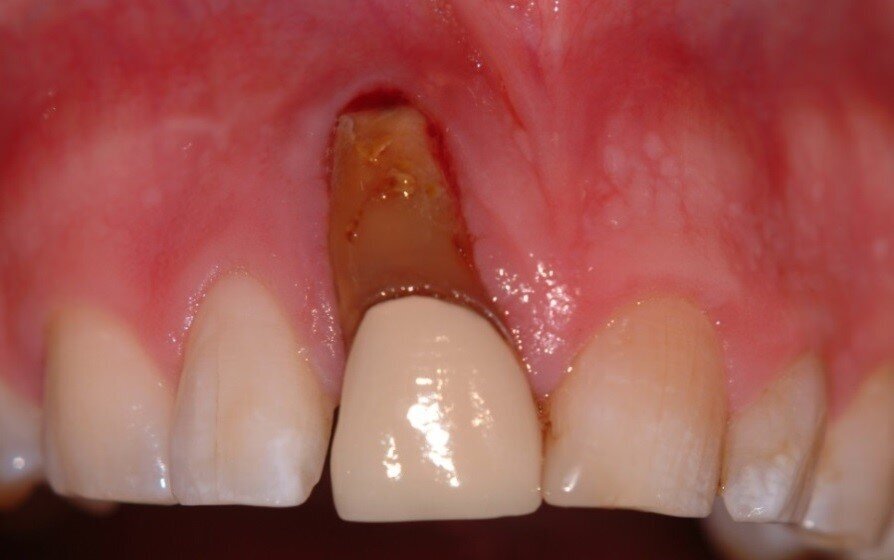
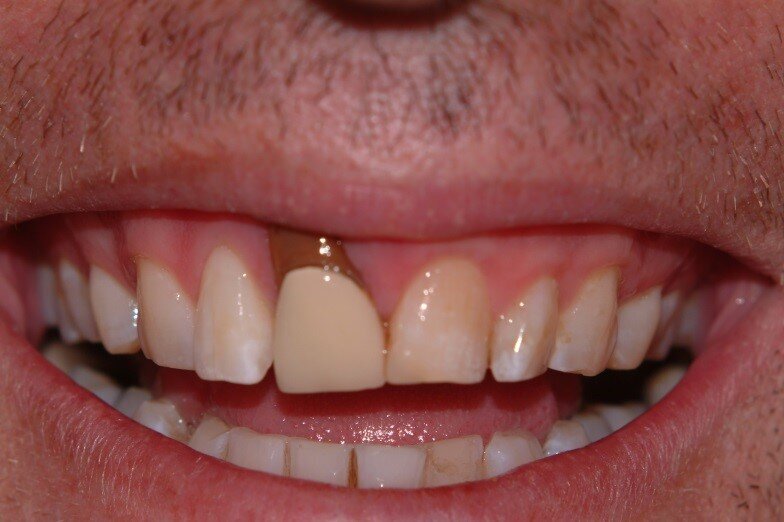
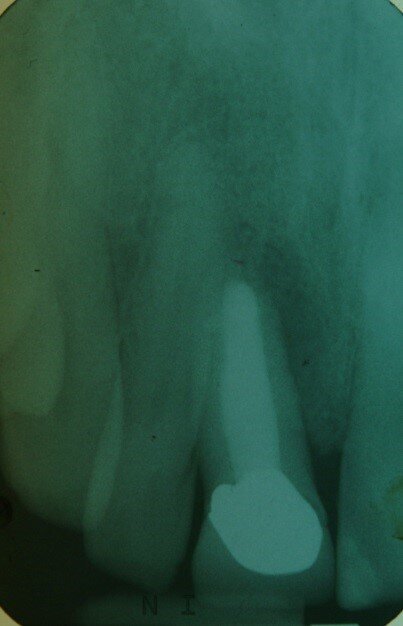
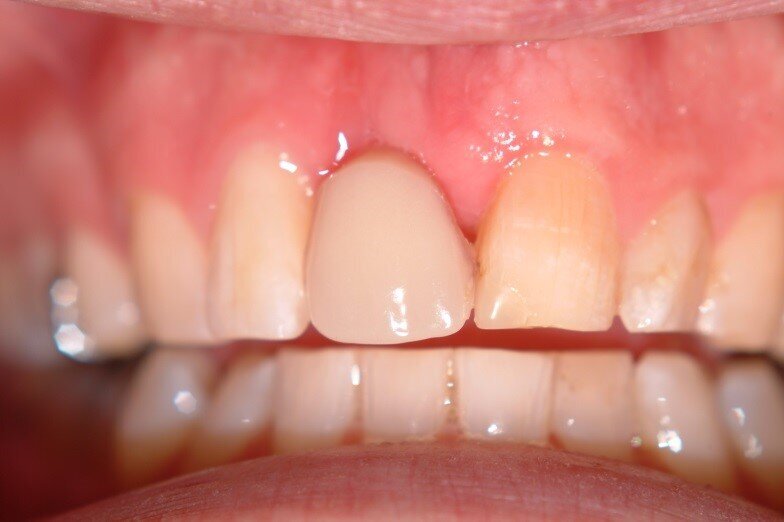
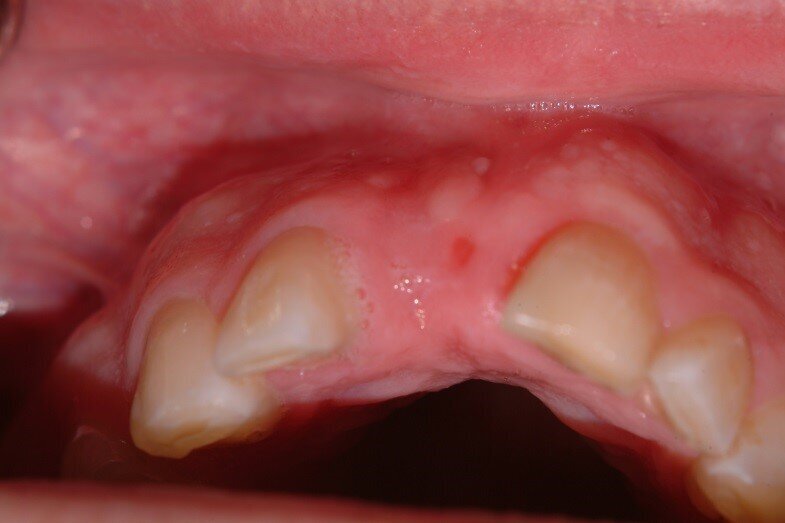
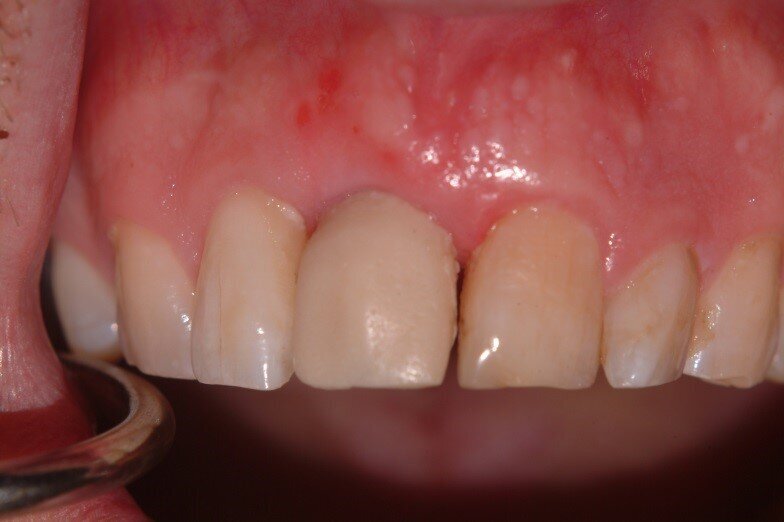
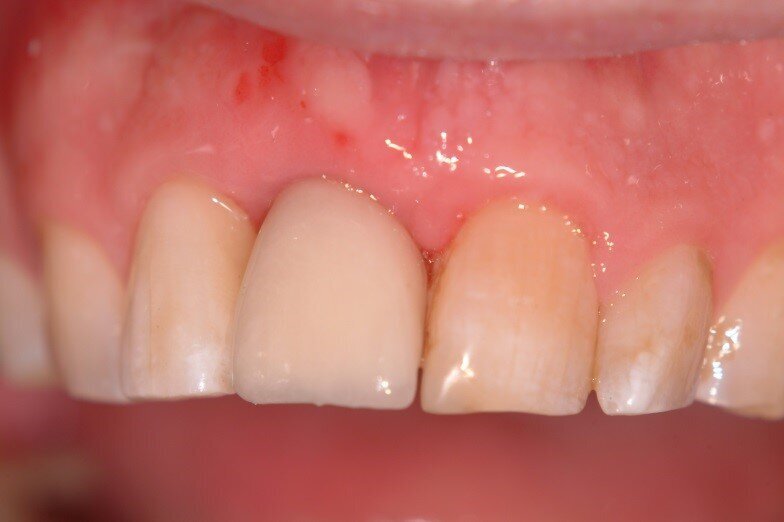
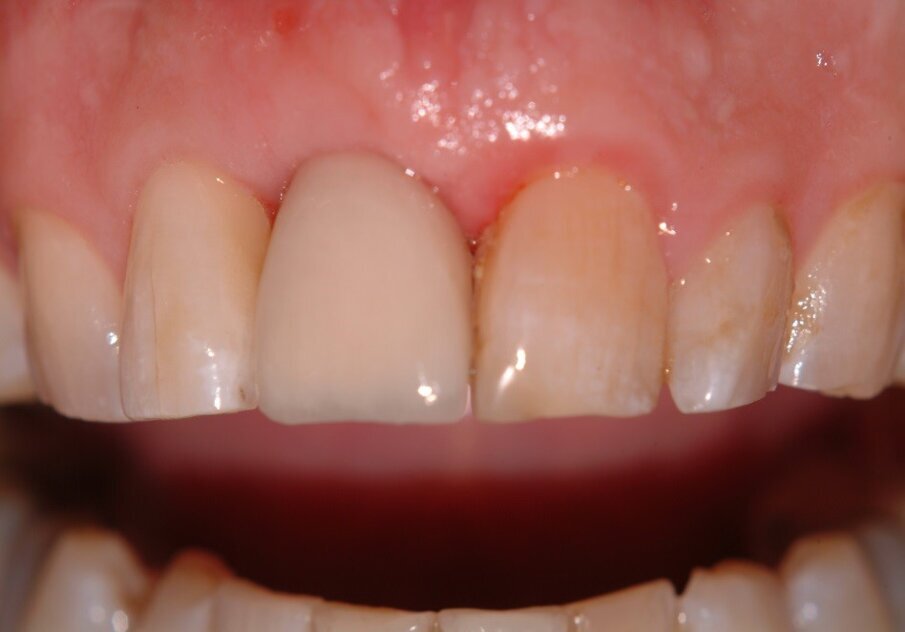
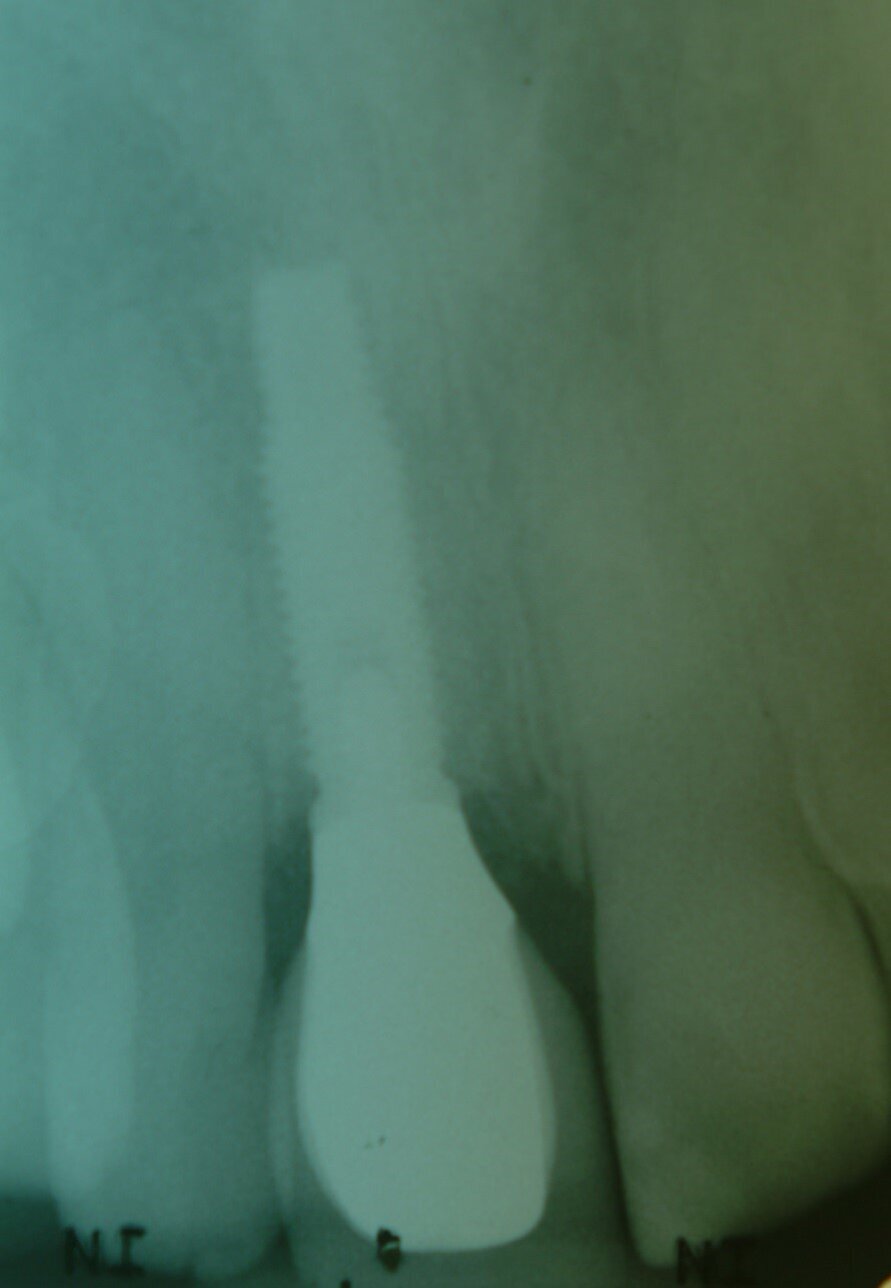
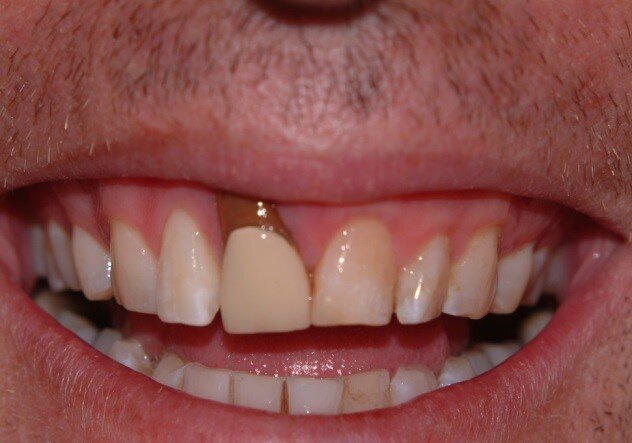
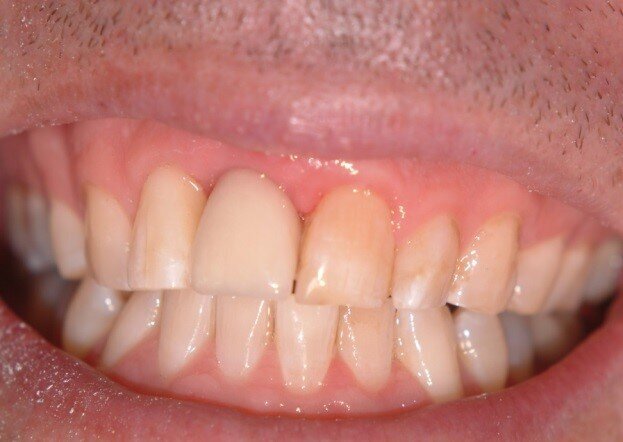
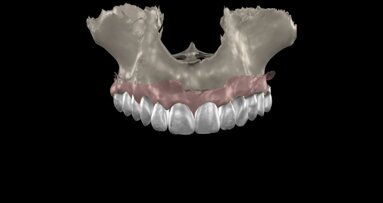
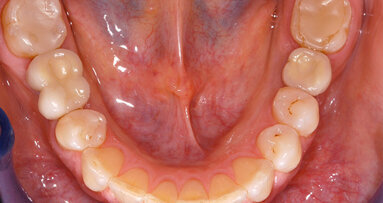
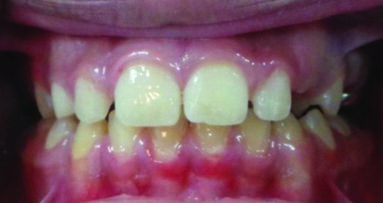
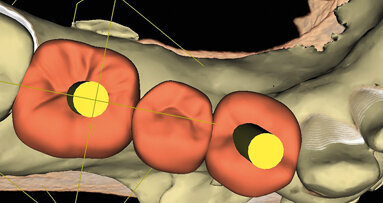
Patient RR was a healthy non-smoking 44 year old male who presented with a complaint of an unaesthetic upper right central incisor with extensive recession showing a large amount of darkened labial root surface. The situation was worsened by a high smile line and a porcelain crown contrasting dramatically with the root colour. He had had periodic swelling at the apical part of the recession over a long period. There was a history of trauma in his teens leading to root canal treatment and a crown, and subsequent apicectomy in his 20s. Clinical examination revealed an otherwise periodontally healthy, well looked-after mouth. (Fig. 1, 2, 3)
Diagnosis was of endodontic failure and possible root fracture leading to loss of labial bone and soft tissue.
With a complex situation such as this, it often beneficial to visualize the end result – in this case an implant supported crown, supported by adequate bone and soft tissue providing gum line symmetry – then to work out “how do I get there from here”?
In this case the treatment plan was essentially divided into 3 stages:
• Rebuilding the lost soft tissue – necessary to close over bone graft materials and give symmetry
• Rebuilding the lost bone – necessary to provide support for an implant
• Replacing the tooth
In detail these involved:
Rebuilding the lost soft tissue
1. Fabrication of a tooth borne immediate partial denture
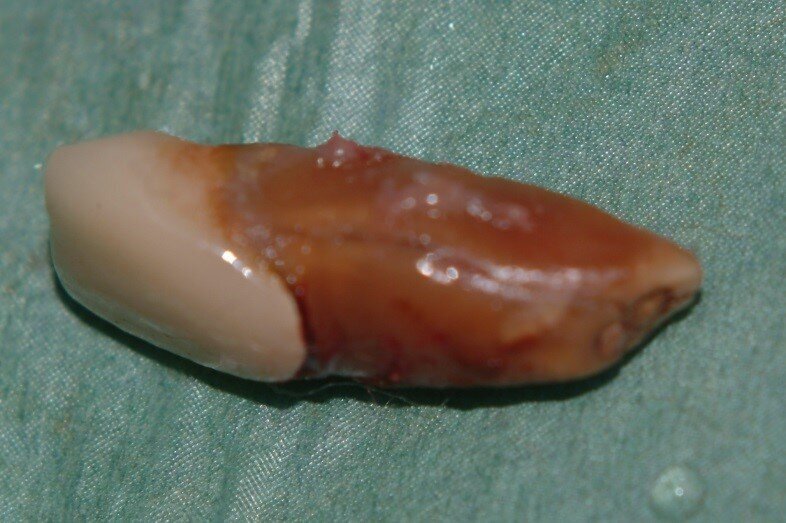
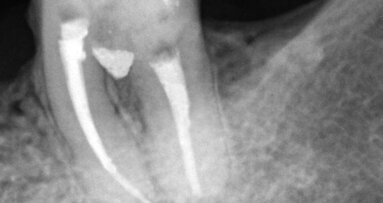
2. Extraction and the split root confirmed (Fig. 4)
3. De-epithelialise the socket and ensure bone bleeding
4. A connective tissue and epithelial graft from the tuberosity – using a distal wedge technique
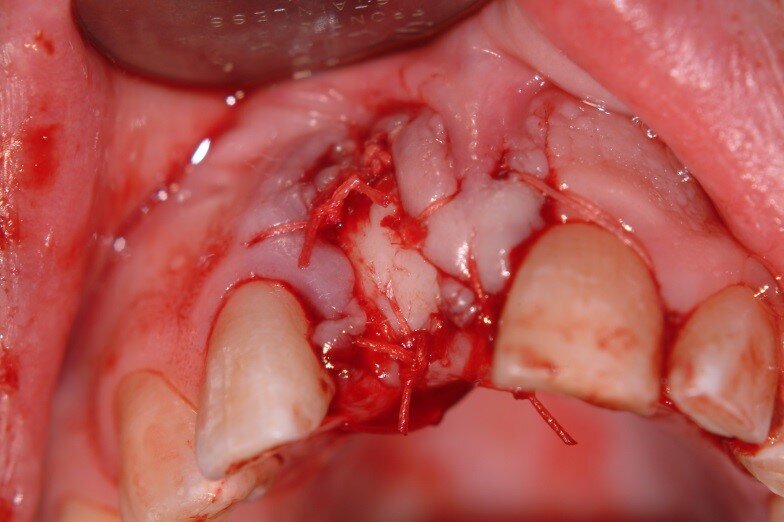
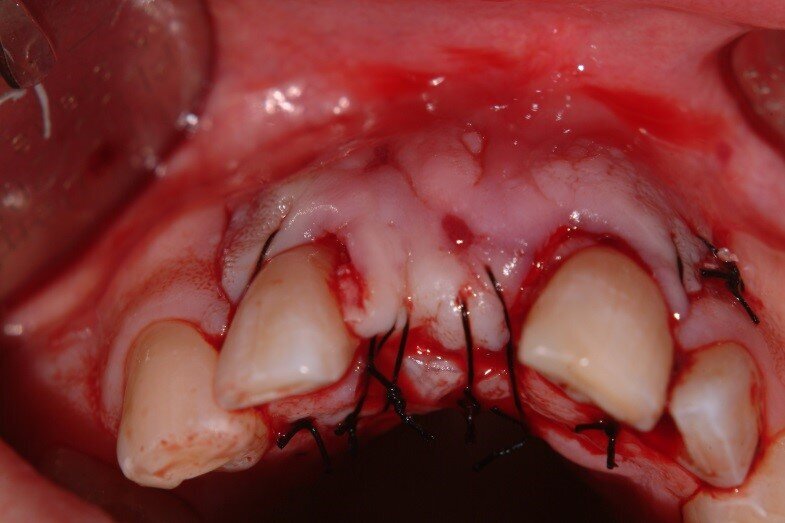
5. Bilateral pedicles using adjacent papilla to cover the connective tissue surfaces of the tuberosity graft (Fig. 5)
6. Fitting and adjusting as necessary the tooth borne immediate partial denture
7. Monitoring of soft tissue healing. Tissue from the tuberosity and adjacent papillae gives a better match than palatal tissue. We are ready to re-enter when incision lines fully closed. (Fig. 6, 7)
Rebuilding the lost bone
1. Re-entry was carried out at 4 months using a full thickness flap for access.
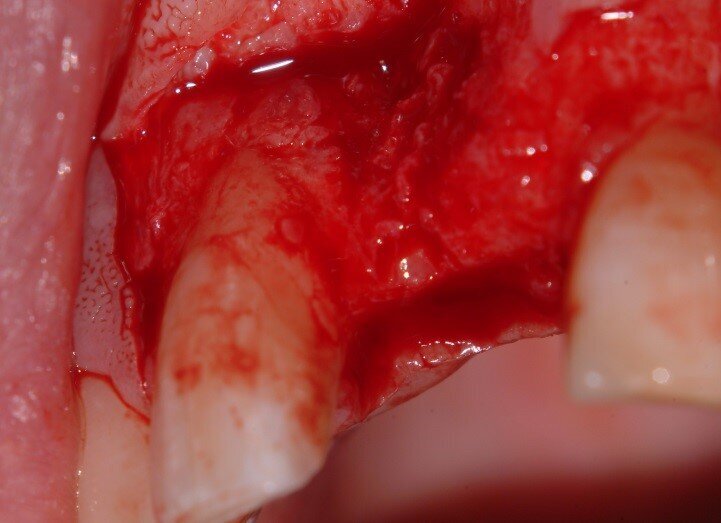
2. Underlying bone was curetted with a Rhodes chisel and a round bur was used on the labially-facing surface of bone to ensure bone bleeding (Fig. 8)
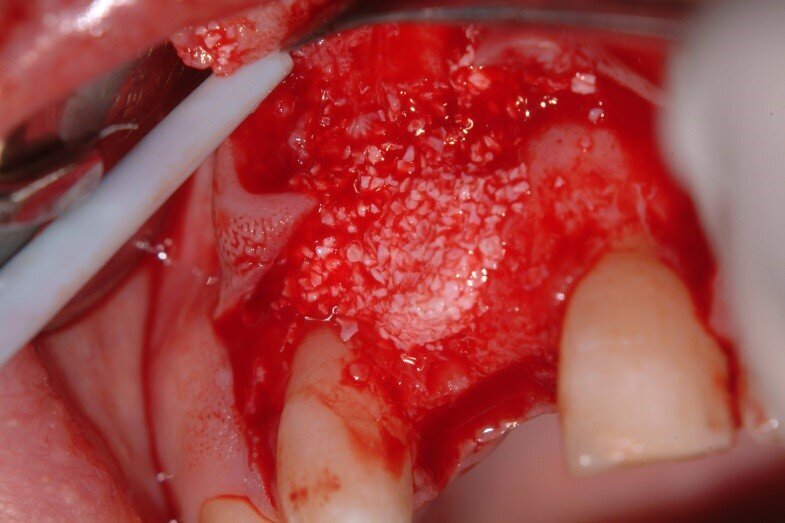
3. Endobon xenograft material (Biomet 3i) was placed after being moistened with blood and saline (Fig. 9)
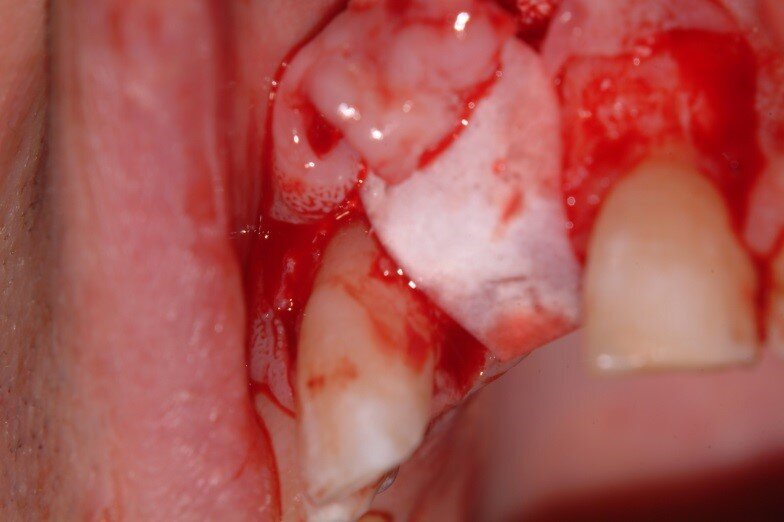
4. OsseoGuard xenograft membrane (Biomet 3i) was trimmed and fitted once it seated passively under the flap (Fig. 10)
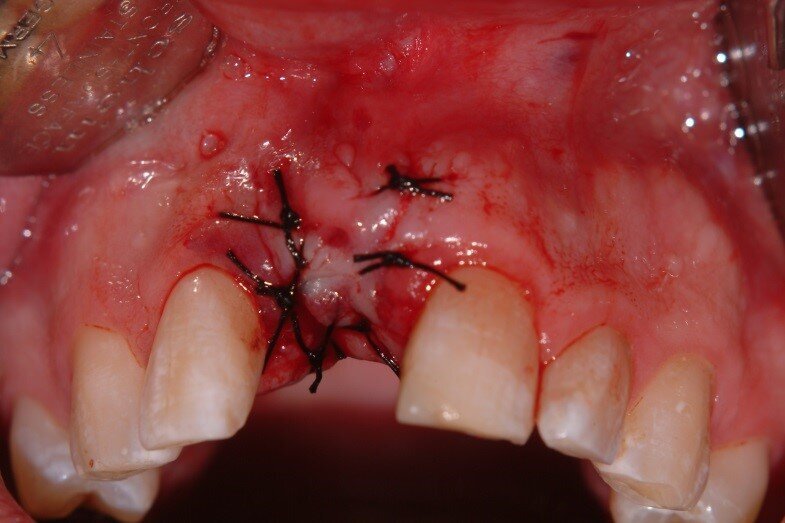
5. The flap was sutured with 4-0 silk to achieve primary closure over the site. (Fig. 11)
6. The partial denture was adjusted and refitted after ensuring there was no positive pressure in the area of the grafted bone.
7. Monitoring of healing. Sutures were removed at 2 weeks and periapical x-rays taken at 2 and 4 months to check for good graft condensation and to ensure there were no voids in the graft material. The timing of implant placement will also depends on bone available beyond root apex position
Replacing the tooth
1. The graft was left to mature for 6 months then a full thickness papillae preserving flap was used to access the site, revealing excellent regenerated bone
2. A 15mm Full Osseotite straight sided external hex implant (Biomet 3i) was placed with an insertion torque of 45Ncm. Because the implant was largely in regenerated bone, immediate restoration was not attempted. No additional grafting material was needed. (Fig. 12, 13)
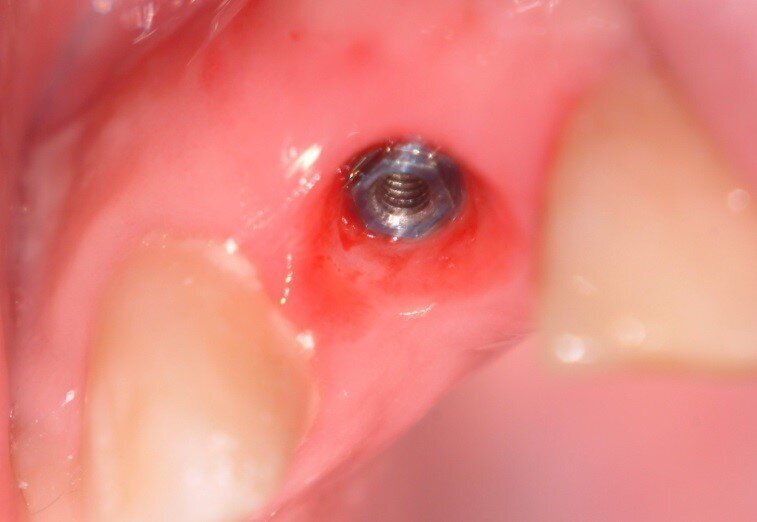
3. After 4 months exposure was carried out using a punch gingivectomy approach.
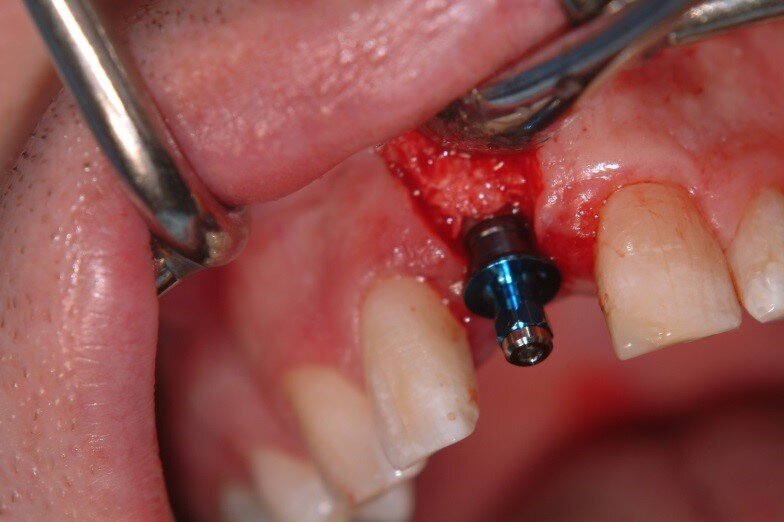
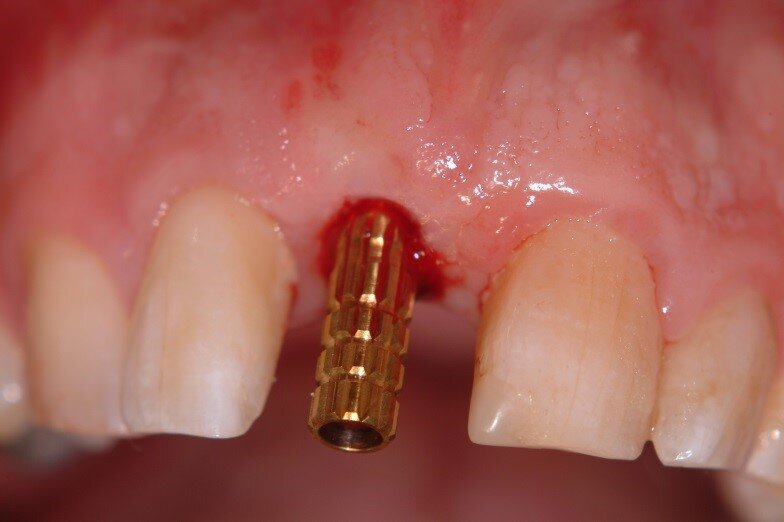
4. A temporary cylinder was seated and a clear crown form was used with cold cure acrylic to fabricate a temporary crown. This was Torqued to 20N/cm and cotton wool and Cavit placed in the access hole. (Fig. 14, 15)
5. 4 Weeks healing was allowed for gingival contour to be developed (a little longer would have been preferred however the patient was moving away from the region) (Fig. 16)
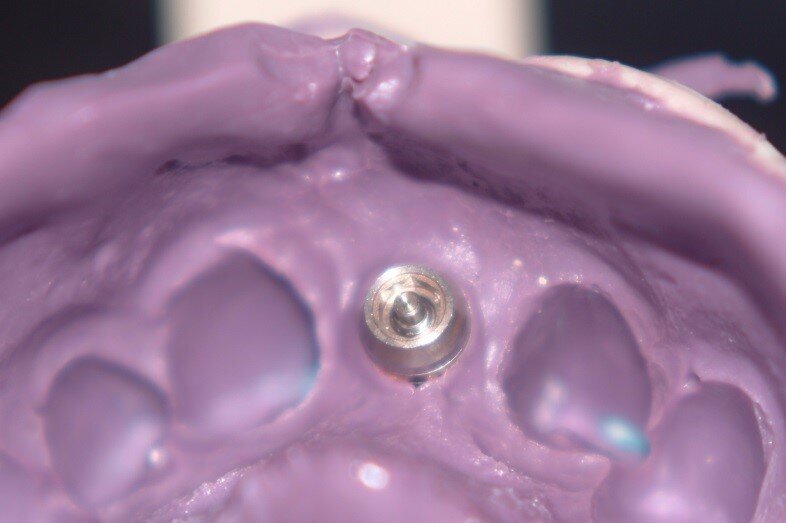
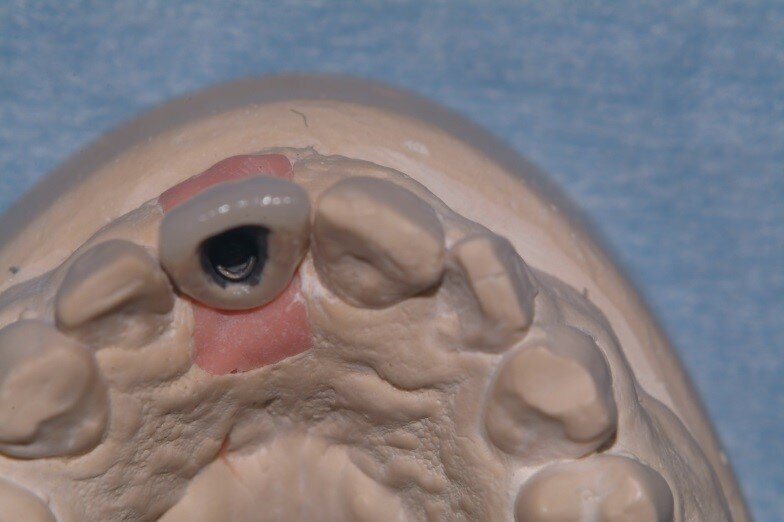
6. Pick up coping impression was taken with Impregum injection into sulcus to capture emergence profile developed with the temporary crown. Occlusal records and shade were taken and agreement was reached with the patient on a midline diastema to improve symmetry. (Fig. 17)
7. The porcelain fused to metal, screw retained crown was tried in, and the fit and occlusion were checked then, after aesthetics had been approved by the patient, a square Goldtite screw was torqued to 32 N/cm and access sealed with cotton wool + composite (Figs 18, 19)
8. A final x-ray was taken and oral hygiene instruction and recall advice were given.
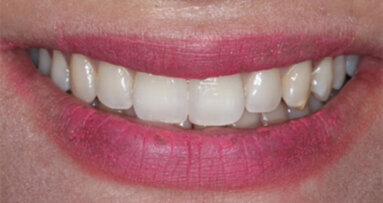
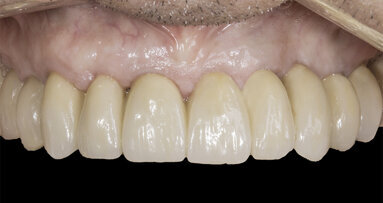
9. The patient returned one year later for a recall examination and x-ray and was still delighted with the aesthetic improvement (Fig. 20, 21, 22)
This case report illustrates the fact that not all tooth replacement problems can be managed by immediate or rapid implant restoration of the lost teeth. While the concepts of immediate replacement and immediate loading of implant prostheses certainly has a place in our armamentarium, it is not applicable to all situations and is certainly a long way from being a panacea. We may all enjoy fast food occasionally, but generally slower, more relaxed fine dining is preferred. It is perhaps appropriate to consider Dennis Tarnow’s maxim “Do one miracle at a time”.
As an oral surgeon and prosthodontist specialising in full-mouth rehabilitation, I have consistently sought to integrate advanced technologies into my ...
In my lecture at this year’s EAO meeting, attendees received an overview of over 50 years of working with implants and why we did it in certain ways back ...
In this article Dr. Thomas Zumstein presents a Neoss implant case that has been in function for more than 11 years. The case shows that long-term success ...
A 28-year-old female patient had the primary complaint of spacing in the upper front tooth region. The patient’s medical history did not reveal any ...
Molar incisor hypomineralisation (MIH) is a relatively common dental defect that appears in first permanent molars and incisors and varies in clinical ...
Part of creating an optimal workflow involves the ability to reliably plan for variables that differ with each patient. 3D imaging gives the clinician the ...
3M Oral Care participated in the Saudi International Dental Conference from 9-11 Jan 2017 held at the Riyadh International Convention and Exhibition Center....
Proper monitoring and maintenance are essential to ensure the durability and health of a dental implant.
DUBAI, UAE: New York University (NYU) in the US has appointed Dr Abdulsalam al-Madani as a professor, making him the first Emirati to hold such an academic...
Female patient, 47 years old, presented with a clinical picture of extensive iatrogenic perforation of the furcation region of the dental element 36 (Figs. ...
Live webinar
Wed. 3 June 2026
9:00 pm UAE (Dubai)
Live webinar
Thu. 4 June 2026
10:00 pm UAE (Dubai)
Live webinar
Mon. 8 June 2026
8:00 pm UAE (Dubai)
Live webinar
Mon. 8 June 2026
9:00 pm UAE (Dubai)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
10:00 pm UAE (Dubai)
Live webinar
Wed. 10 June 2026
7:00 pm UAE (Dubai)
Live webinar
Wed. 10 June 2026
10:00 pm UAE (Dubai)
Nacho Fernández-Baca DDS, MSc



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس













































To post a reply please login or register